Breast Cancer: Let’s Not Settle for Less
October 19, 2018 • community
School of Public Health & Texas Center for Health Disparities Community Blog
Whether through our own experiences or a loved one’s, breast cancer can be scary. As a community, we have worked hard in the last few decades to increase awareness and knowledge regarding breast health. We started recognizing October as the breast cancer awareness month to remember those who lost their battle to this disease, to celebrate the courage and strength of survivors, and to encourage others to get regular screening for early detection and treatment. It is also hard to miss the pink ribbon symbol at grocery stores, doctor’s offices, online among other avenues, reminding people that breast health is important and early detection through screenings can help save lives.

Through these efforts, we have made some progress. There has been a 24% reduction in breast cancer-related deaths between 1999 to 2015.1 While this is great news, it is time we ask ourselves, are we doing enough? How can we make this better? The first step in answering these questions would be to reflect on our current status. How much do women know about breast health and where do they get their information?
In 2015, we attempted to seek some answers and assessed breast health knowledge among 43 women participating in a breast health educational event, and 91 additional women who attended a screening session in Tarrant County. The majority of women in our study ranged between 40-59 years of age and identified as either African American/Black or as Hispanic/Latina. Our goal was to explore if women were able to identify breast cancer related symptoms and if they were aware of factors influencing their risk of breast cancer. The graphs below show a snapshot of our findings.
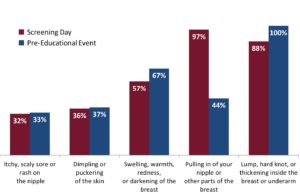


Our results demonstrated that women knew very little about non-lump related symptoms and there was an inconsistency in overall breast health knowledge. This prompted us to look into where women were receiving their information. What do guidelines suggest? We learned very quickly that many versions of breast health related information exist online, and more surprisingly, they do not always agree with one another. Even after shortlisting reliable sources such as the Center for Disease Control and Prevention, Komen Foundation, American Center Society, and National Breast Cancer Foundation, we found inconsistencies in recommended guidelines. First, with the exception of breast cancer symptoms listed by CDC, information in all other sources listed (see figure 4) were written above the fifth grade level which goes against the health literacy principles2 regarding the use of plain language. Health information must be written at fifth grade level or below to ensure that people can read, understand and act upon the information.
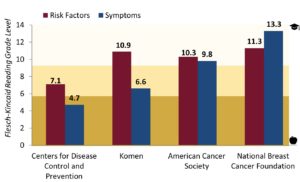
While the four organizations listed agreed upon risk factors, symptoms, and the lack of reliability of self-examination, they disagreed with regards to when women should initiate screening (40 versus 45 versus 50 years of age). They also disagreed on screening frequency and method of screening.
These inconsistencies in guidelines and preventative measures for breast cancer between sources may create confusion. In turn, this may obstruct women from receiving necessary clinical breast exams and mammograms, resulting in delayed diagnosis and treatment. They may wonder, ‘If I am at 42 years of age, should I start going for mammogram? Am I already late? Or should I wait till I am 45 or 50 years of age? What is the correct answer?”
There is a need for organizations to revisit their breast health guidelines and agree upon the necessary course of action. It is also vital to ensure that women can understand factors related to breast health, are encouraged to monitor their breast health, and are knowledgeable about available healthcare services. This can only be accomplished through simple, clear and consistent messaging.
It is true that we have come a long way in our battle against breast cancer and reducing breast cancer-related deaths; 24% in about a 15-year span is an accomplishment! Let’s not settle for 24%! By bringing organizations and communities on the same page with regards to breast health, we can continually improve survival rates – let’s think about all the lives we can save!
You can read Texas Community Profile3 published by the Susan G. Komen Foundation to learn more about breast cancer rates in the state of Texas and respective counties. This report helps identify high-risk populations in our local communities and presents a cancer control plan. If interested in joining the fight against breast cancer, visit Susan G. Komen, Cancer Care Services websites or other local organizations to learn more about ways to get involved.
Blog Author: Shlesma Chhetri, MPH, CPH
Acknowledgements:
Emily Spence-Almaguer, MSW, PhD
Katherine Cantu Anguiano, MPH, CPH, CHES
Marcy Paul, PhD
Anjali Desai, MPH
Misty Wilder, BS
Funding for this evaluation was supported by Susan G. Komen of Greater Fort Worth community grant awarded to the Greater Mount Tabor Christian Center to support efforts of the Tarrant County Cancer Disparities Coalition under UNTHSC IRB# 2015-136: Breast Cancer Screening Day Evaluation. Research reported in this presentation was partially supported by the National Institute on Minority Health and Health Disparities Exploratory Centers of Excellence of the National Institutes of Health under award number P20MD006882.
The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Reference:
1Centers for Disease Control and Prevention. (2015). United States Cancer Statistics: Data Visualizations. Retrieved from https://gis.cdc.gov/Cancer/USCS/DataViz.html
2We Heart Health Literacy. (2018). Plain Language. Retrieved from https://medium.com/wehearthealthliteracy/tagged/plain-language
3Susan G. Komen Foundation. (2015). Community Profile Report 2015. Retrieved from https://ww5.komen.org/uploadedFiles/_Komen/Content/What_We_Do/In_the_Community/Assisting_Community_Health_Needs/Texas%202015%20Community%20Profile%20Report.pdf
Research reported in this publication was supported by the National Institute On Minority Health And Health Disparities of the National Institutes of Health under Award Number U54MD006882. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.

Social media