Building Bridges Program
WHO ARE REFUGEES?
Refugees, as per U.S. Citizenship and Immigration Services, are persons living outside their country of origin who are forced to leave their homes due to fear of persecution based on their race, religion, nationality, or membership in a particular social/political group. Approximately 70,000 refugees are resettled in the USA each year.
Click here to view the Refugee Screening Process
PILOT PROJECT
The Building Bridges Initiative began in 2010 with intramural funding from the University of North Texas Health Science Center. This initiative- a partnership with Texas Refugee and Immigrant Women’s Association (TRIWA) trained refugee women, representative of four refugee groups, as Community Health Workers (CHWs). The trained CHWs facilitated focus groups to identify health concerns of women from their communities. The group results indicated most women lacked regular health care and faced great obstacles in securing medical home.
WORKING MODEL
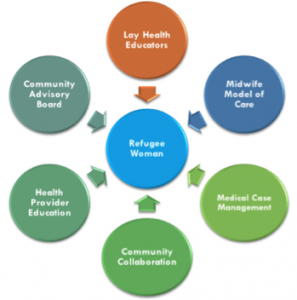
Refugees face health problems that originate from the conditions of their home country, develop during their migration experiences, or emerge after resettlement in the United States. Building Bridges Program, a Cancer Prevention and Research Institute of Texas (CPRIT) funded three year community based intervention program that aims to address cultural and linguistic barriers to preventative health screenings through an integrated and multi-prolonged approach, which includes:
Lay Health Educator Outreach and Education
Midwife Model of Care
Medical Case Management
Community Advisory Board
WHY REFUGEES?
NEED FOR MAMMOGRAPHY & CERVICAL SCREENING AMONG REFUGEE WOMEN
There is insufficient literature regarding refugee health, health risks and preventive behaviors and refugee-specific cancer incidence and prevalence rates. The most studied populations are those that migrated many years prior, such as the Vietnamese and Cambodian. There is evidence, however, that immigrants, including refugees, are medically underserved. For example, a study of 915 ethnically diverse immigrant women in New York City found that women in the US for 10 years or less were significantly less likely to have had a mammogram within the past two years compared to non-immigrants. Similarly, a study of data from the 2000 National Health Interview Survey found that immigrant women in the U.S. are less likely to receive screenings for breast and cervical cancer compared to non-immigrant women in the United States within the first ten years of migration. There are significant disparities between immigrant and non-immigrant women. Studies of refugees in both early and several years post-resettlement have shown inadequate uptake of cervical screenings and mammograms. A study of Bosnian, Cuban and Vietnamese refugees in Texas found that 86% of women never had a mammogram compared to 33% of American women of the same age, and only 24% had a pap exam in the previous three years. A recent (2011) study of South Asian immigrants found one-third never had a mammogram and only one-third had a previous pap exam.
NEED FOR HEPATITIS B EDUCATION AND VACCINES
According to the National Cancer Institute, Asians and Pacific Islanders in the United States have higher rates of liver cancer compared to non-Hispanic whites. The hepatitis B virus (HBV), responsible for up to 80% of liver cancers in the United States, is endemic to many refugee-producing countries in Asia and sub-Saharan Africa. In 2010, 376 refugees arrived to Texas with chronic HBV Infections, of those 50% were from Burma, 11% from the Congo, 9% from Somalia, and 4% were from Bhutan. Another 63% were susceptible to the infection. The Centers for Disease Control and Prevention recommends the hepatitis B vaccine series for unvaccinated adults at risk.
NEED FOR COLON CANCER SCREENING AND EDUCATION
There is limited research concerning refugees and their need for colon cancer screenings, as well as their familiarity with colon cancer. Despite this, colorectal cancer (CRC) remains the fourth most common cancer type among men and women worldwide. The literature reveals that the longer refugees and immigrants live in the United States, the more likely they are to receive screening. For example, researchers found a 7% increase in the odds of having Fecal Occult Blood Test (FOBT) screening for each additional year of U.S. residency. Flexible sigmoidoscopy/colonoscopy screening increased 39% with every 5 years of residency. Nevertheless, the risk for developing colon cancer may increase during this period. According to the American Cancer Society, the five year survival rate for colon cancer is significantly higher during Stage I at 74%, compared to Stage IV of colon cancer, with a 6% five year survival rate. In another study, researchers surveyed 32,440 participants and found that foreign birthplace influenced late access to care for colorectal cancer, contributing to a decreased rate of survival for people born outside the United States. Education and early screening efforts are imperative to helping refugees understand what colon cancer is, become familiar with the screening process, and learn how to seek help early if cancerous cells are found.

Social media