School of Public Health
Category: community

January 11, 2022 • community
Guest blog article by Linda Fulmer, BSW, MEd Executive Director, Healthy Tarrant County Collaboration Healthy Tarrant County Collaboration (HTCC) has been working to address healthy food access in underserved neighborhoods for a few years now, and after reviewing the Baltimore City’s Food Environment: 2018 report, we wanted to do the same kind of study for…

November 23, 2020 • community
As the holidays fast approach and 2020 continues to give us a run for our money, many people are feeling the effects of pandemic fatigue. Pandemic fatigue occurs when people grow tired of practicing measures meant to slow the spread of COVID-19, such as social distancing, wearing a mask, staying away from large gatherings, etc.…

October 25, 2020 • community
By now we are all intimately familiar with the horrific events that have occurred in 2020. It has been a year full of multifaceted injustices ranging from the outrageously high COVID-19 death toll that has disproportionately affected communities of color, to the violence and deaths that have resulted from police brutality. There have been substantial…
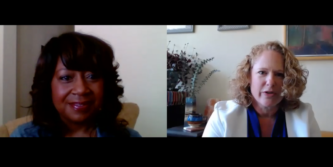
March 30, 2020 • community
In this video blog, we will discuss some community groups who are particularly vulnerable as a result of COVID 19 shelter-in-place orders. We will also hear about how community organizations are quickly pivoting their work to respond to these urgent needs. During this video we speak to: Ms. Leah King Chief Executive Officer United Way…

July 19, 2019 • community
School of Public Health & Texas Center for Health Disparities Community Blog Something happened!!!!! The sounds I awoke to coming from the living room were screams. I always had intense dreams, but I know this wasn’t one of them. I knew something bad had really happened. A few weeks earlier, my mom found out that…

Social media