TCOM, PA students comply with COVID social distance rules while fine tuning their skills via the HSC Simulation Center
By Diane Smith
HSC Fort Worth has taken virtual learning to new levels during COVID-19.
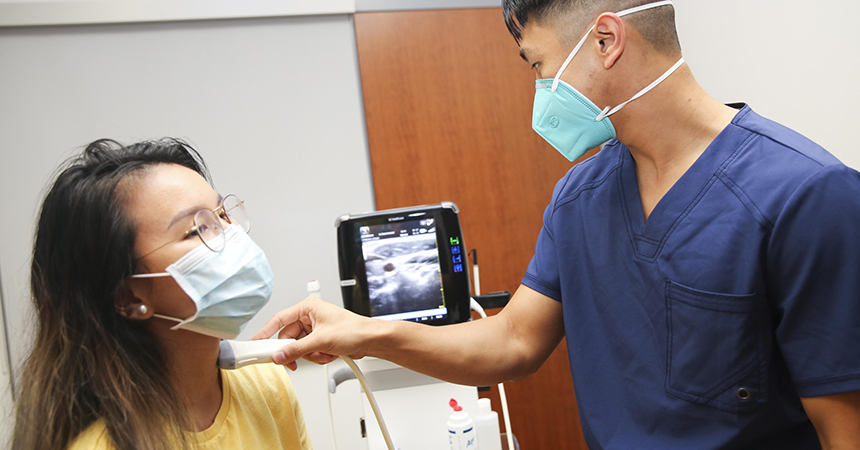
Consider, for example, medical students at the Texas College of Osteopathic Medicine who must master ultrasound technology to better identify the diseases that ail patients.
At TCOM, students gain these skills while also learning to teach their peers. Earlier this year, about 20 to 30 students worked to become teaching assistants in the ultrasound training program directed by John O. Gibson, MD; FAAFP, DIMPH, CTropMed and Assistant Dean, Rural Medical Education.
But the global pandemic interrupted in–person ultrasound training for large groups of students. Dr. Gibson’s group at The University of North Texas Health Science Center’s Simulation Center helped to bridge an emerging education gap.
COVID-19 is forcing colleges and universities to create new virtual learning strategies. In this climate, the HSC Simulation Center is figuring out ways to deliver critical hands-on training to students in creative ways.
“When COVID hit, we had students who were used to coming to the Sim Lab who still needed to have some experiences – explorational learning experiences – and that stopped,” said Karen Meadows, MSN, RN Director of the HSC Simulation Center.
The Simulation Center, also referred to by faculty, students and staff as “The Sim Lab,” has been accommodating students online and with in-person activities that delivered learning with safety measures in place.
TCOM’s ultrasound training is just one example. TCOM faculty needed to train teaching assistants in ultrasound techniques even as social distancing was underway. A course was developed and delivered remotely with equipment from HSC’s Simulation Center.
“For the first two months that we were not allowed to be on campus, we were doing Zoom calls. Dr. Gibson was doing demonstrations over the internet and we were trying to learn as much as we can,” said Vincent Hua, a second-year TCOM student and ultrasound teaching assistant.
This fall semester Hua and other students spent most of their learning off-campus – out of about 60 hours of learning a week about three to four are on campus. Some of those campus hours are spent learning to use ultrasound technology in small groups of about three led by a teaching assistant.
“There are some skills you have to learn in person,” Hua said, explaining that the smaller groups adhere to social distancing rules. “We are minimizing the risk of spreading COVID-19.”
Working to solve problems
Meadows said the Simulation Center is solving problems and finding new ways to deliver simulation training.
The Simulation Center has a three-person staff that includes Meadows, Tony Martinez and Josh Christian. Together they have tackled several issues, including providing a suture lab for students in HSC’s graduate Physician Assistant Studies program.
“Normally, they would come to campus for that and we would set up all the equipment and everything that they need,” she said.
But PA students couldn’t come to campus.
The team collaborated with faculty to offer suture practice at home. Students received multi-layer synthetic suture pads and suture kits so they could practice techniques at home. When they return to campus, they can show their skills.
Meadows said Martinez made realistic-looking suture or “human” skin that can be used to practice stitching a laceration.
“It basically takes the lab home,” Meadows said. “It’s the same skills. It’s the same class they would have done on campus. The innovative part was finding a way to take the suture lab out to the students instead of the students to the Sim Lab.”
Mareah Lucio, a second-year PA student, was in a virtual class that practiced stitching wounds at home last summer. For the class, Clinical Integrated Medicine, Lucio used her laptop, cellphone camera and suture tools to practice alongside dozens of other students in a virtual classroom.
Lucio said this fall much of her learning continues to be online and she adapting to the challenges.
“It’s difficult, but I feel like PAs – the whole profession – we were made to be flexible,” Lucio said. “We are made to adapt. I think it is practice for what we are going to have to do in the future.”
Jamie Park, M.S., M.P.A.S., PA-C, Assistant Professor for the School of Health Professions, said she will continue using some aspects of these virtual lessons in future classes, including turning in video of their suturing.
“We will have students continue to record themselves and then upload it so we can correct their techniques,” Park said. “It was such a success. It allowed us to do it slowly versus having 75 students in a room at once and trying to correct them.”
The Simulation Center also purchased the Oxford Medical Simulation program, a scenario-based virtual reality program that allows PA students to practice patient visits. Students can practice treating and interviewing patients about their ailments in a virtual clinic.
The online tools allow for a near complete clinic experience, Meadows said.
“They can do almost everything,” she said. “They can grab a stethoscope and listen. They can take temperature. They can ask questions.”
The Simulation Center also established an online standardized virtual patient encounter program, said Christian, the center’s Simulation Administrative Specialist.
During patient encounters, standardized patients – actors who play the role of a patient – and medical or PA students interact. The standardized patients are assigned a specific ailment to portray or specific medical case that they are acting, he said.
Those patient encounters used to take place on campus, but person-to-person sessions were no longer viable because of COVID-19. Telehealth technology helped take the sessions to the students’ homes, she said.
“We took what was happening on site and we figured out how to put it online,” Meadows said, explaining that it looks similar to a meeting on Zoom.
New learning opportunities
Meadows said they will add more educational support on and off campus with funding provided by the Coronavirus Aid, Relief and Economic Security Act (CARES).
Meadows and others at HSC said dealing with the pandemic’s educational obstacles made their simulation program stronger.
“For me, what I am most proud of for this department, is that during COVID we stayed relevant, we found new solutions for problems, we found new ways to do things that hadn’t been done before and we just continued working it until we found a way to make it happen.”
At TCOM, peer-to-peer teaching is creating a new learning experience.
“I believe it is a really valuable experience to learn from someone you may feel more comfortable with or maybe someone you don’t see as above you,” Hua said.
Even though COVID-19 changed the learning environment for medical students, new lessons emerged.
“We are missing out on some things, but we are learning to face these challenges head on,” Hua said. “We are getting experience that other students don’t get. I’m excited to see how it affects our education and I hope to use this experience to what I do in the future.”



![Uyen Sa Nguyen Scaled[58]](https://www.unthsc.edu/newsroom/wp-content/uploads/sites/16/Uyen-Sa-Nguyen-scaled58-145x175.jpg)


Social media