Pharmacists are fighting on the front lines of the COVID-19 pandemic
By Diane Smith
Managing medicines, counseling patients, giving flu shots and checking glucose is the everyday work of pharmacists.
But as the nation fights coronavirus, the work of these healthcare professionals has been expanded by the federal government to include COVID-19 testing. It’s a move that makes sense to pharmacy experts.

“This is another moment in time where pharmacists are proving that they are willing and able, and they have the education to do whatever the healthcare community needs them to do,” said Emanuel George, PharmD and Associate Dean of Student Engagement and Alumni Affairs at the UNT System College of Pharmacy.
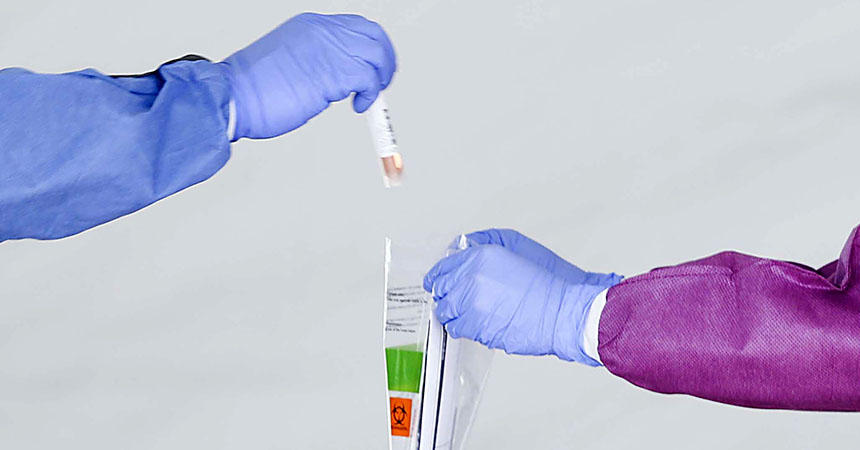
On April 8, the federal government announced that licensed pharmacists can order and administer COVID-19 tests approved by U.S. Food and Drug Administration.
“Giving pharmacists the authorization to order and administer COVID-19 tests to their patients means easier access to testing for Americans who need it,” said U.S. Health and Human Services Secretary Alex Azar in a statement. “Pharmacists play a vital role in delivering convenient access to important public health services and information.”
When the disease emerged in the United States, pharmacists were among the first answering questions, Dr. George said. They continued to be a resource even as cities followed shelter-in-place, social-distancing guidelines and began limiting contact with the healthcare system.
“They are answering dozens, if not, hundreds of questions per day,” Dr. George said, explaining how pharmacists can be found helping the public from behind Plexiglas counters, drive-thru windows and the computer screens of telemedicine.
Dr. George said people struggling with sniffles, coughs or fevers are asking pharmacists: “Are my symptoms COVID-related?”
Pharmacists also are serving alongside doctors and nurses as part of intensive care units determining which medications and therapies will fight a disease that attacks the respiratory system.
“Pharmacists are on frontlines in multiple types of practice settings – from hospital settings to community clinics, where they are seeing patients one-on-one,” Dr. George said.
Pharmacists on the frontlines

Dr. Crystal Howell, Assistant Professor at the College of Pharmacy and an infectious disease pharmacist, said pharmacists who work in multiple specialties in hospitals – including critical care, infectious diseases and emergency medicine – are working together to optimize care of patients with COVID-19 and to protect their healthcare colleagues.
“They are considered essential employees,” Dr. Howell said. “They are constantly being exposed.”
Dr. Marian Gaviola, an ICU pharmacist, said pharmacists were already working in inter-professional teams with doctors and nurses when the pandemic arrived.
“We have had to be stronger together and be able to speak to our expertise right now,” Dr. Gaviola said. “No one profession can tackle it on its own.”
How pharmacists approach medication on the frontlines can save lives, Dr. Howell said. For example, to better protect nurses, pharmacists might recommend a dosage that is given once instead of multiple times, she said.
This strategy decreases risks and saves on equipment because nurses don’t have to put on protective gowns, masks and eye protection so many times, Dr. Howell said.
Pharmacists are helping figure what medicines might work against the virus and resulting ailments that surface as patients fight COVID-19. Pharmacists are analyzing medications and steroids that can help with respiratory complications because the virus affects the lungs and can lead to pneumonia.
Dr. Gaviola said pharmacists are planning how to use medications amid the unknowns of a crisis.
“What do we do when drugs that we need to use aren’t available?” she said. “How do we make sure we are using the right drugs for the right people?”
Dr. Gaviola said COVID-19 presents different issues. For example, deciding which medications can be used to sedate patients on ventilators, or how to prevent and treat clots that occur at the same time.
How medications are delivered also has to be considered so they don’t end up spreading the disease, Dr. Gaviola said. These questions are considered when trying to decide how to deliver breathing treatments to COVID-19 patients, she said.
“What kind of inhaler should you use in a patient who has COVID-19?” Dr. Gaviola asked.
‘We want to find a solution’
Pharmacists said they have a common desire to stop the spread of COVID-19.
“This falls within our realm of expertise and passion,” Dr. Howell said. “We want to find a solution.”
Dr. Howell said pharmacists are reading and analyzing research to find the best solutions for their patients. They’re also working to come up with alternatives to secondary medication shortages caused by the pandemic.
Many pharmacists are writing policies or local guidelines to share their findings about medicines being used or research trials. There was even a pharmacist author on the recent NIH treatment guidelines, demonstrating that pharmacists are on the front lines locally and nationally.
The motivation is simple, Dr Howell explained: “We are healthcare professionals. When we see people who need help, we are going to go.”
The pandemic is an opportunity to learn in real time, and experts say it is shaping the future of healthcare. It is also a chance to prepare for future health crises.
“People are scared,” Dr. Howell said, adding that it is important to keep hope. “We have to learn from this experience. We have to learn and prepare for the future.”

![Uyen Sa Nguyen Scaled[58]](https://www.unthsc.edu/newsroom/wp-content/uploads/sites/16/Uyen-Sa-Nguyen-scaled58-145x175.jpg)



Social media