Monitoring health from a patient’s home
For Yvette Clayborn, the past year was a blur of hospital rooms.
Hypertension and other health issues forced the Fort Worth woman in and out of hospitals for most of 2014. She was always worried, unsure when headaches or fatigue signaled a dangerous spike in blood pressure.
“It is exhausting,” Clayborn, 51, said wearily.
Today, Clayborn hopes a visionary new program conducted in a partnership between UNT Health Science Center and CareCycle Solutions, LLC, can end the hospital merry-go-round. The program uses patient-monitoring equipment that allows nurses to remotely monitor patients in their homes, thus reducing hospital readmission rates and increasing quality of life.
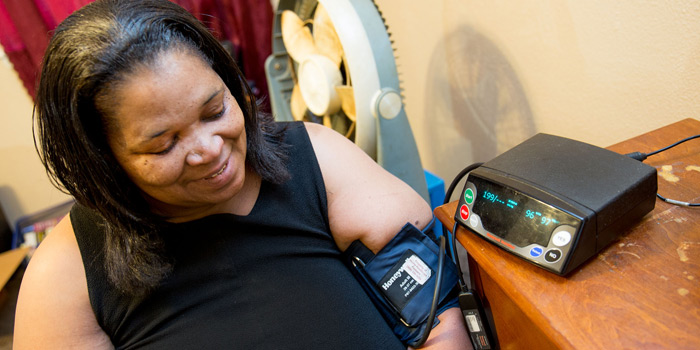
Every morning at 10 a.m., a hospital-grade telemonitor – a digital box connected to a scale, blood-pressure cuff and heart-rate monitor- alerts Clayborn with an audible sound that it’s time to measure her vitals. “Good morning,” the box’s digital screen greets her as she straps the cuff onto her arm.
Her weight, blood pressure, heart rate and oxygen levels are transmitted to an experienced critical care nurse at CareCycle Solutions, a company that specializes in helping people manage their chronic health conditions. If Clayborn’s measurements raise red flags, the nurse can call Clayborn to discuss what is occurring – or, if necessary, contact her primary care physician.
“I like it because I’ve talked to the nurse almost every day,” Clayborn said. “Sometimes, she just checks in on me. It helps me to ask questions to someone who knows what is happening to you.”
Clayborn’s primary care physician, Didi Ebert, DO, who practices at UNT Health, said the program helps her keep track of Clayborn’s health without requiring her to travel for an appointment.
“When she does have an appointment, we can spend more time focusing on her big-picture health needs because issues like her blood pressure have been monitored,” Dr. Ebert said.
Funded by a grant from the Centers for Medicare and Medicaid Services, the program hopes to enroll 715 patients by September 2016. The United States faces a chronic disease crisis, spending more than $17 billion each year on avoidable hospital readmissions.
“Improving quality and reducing the cost of health care is a national priority,” said Brad Cannell, PhD, Assistant Professor in the UNTHSC School of Public Health, who manages the project. “We hope that this public-private partnership will demonstrate one method for doing both.”





Social media