Lessons from the battlefield
November 27, 2017 • Physician Assistant Studies
By Alex Branch
The training to provide life-saving trauma care in the chaotic conditions of a battlefield was once limited to military medical personnel.
But in an era of terrorism and mass shootings, some of those skills can today help civilian medical providers and lay people save lives.
That’s why Jeffrey Mott, DHSc, PA-C, recently showed students at UNT Health Science Center some of the lessons he once taught military medical providers preparing for deployment to combat, such as how to tie effective tourniquets or treat penetrating chest wounds.
The skills learned by about 30 members of UNTHSC’s Physician Assistant Surgical Organization help prepare them to be first responders at critical incidents or work in emergency rooms after large disasters.
“All of our members have an interest in orthopedics or trauma, and Dr. Mott offers a great skills clinic for us to get hands-on training,” said Dani Lutes, a 2nd-year PA student. “We had no trouble filling up the spots in this course because these are skills we want to learn.”
Tactical Combat Casualty Care (TCCC) was first implemented in the 1990s by U.S. Army Special Operations, and eventually by all the military branches after the Sept. 11, 2001, attacks and subsequent war on terrorism, said Dr. Mott, Assistant Professor and Director of Clinical Education for the Physican Assistant Studies Program. TCCC is credited with saving the lives of thousands of U.S. military and coalition personnel in the Iraq and Afghanistan conflicts by providing prehospital critical care to the wounded.
In more recent years, elements of combat casualty care have trickled into the civilian world, a point Dr. Mott emphasizes by showing students images of first responders and bystanders using tourniquets to stop bleeding and save lives in the aftermath of the 2013 Boston Marathon bombing.
A person can bleed to death in five minutes, he said.
“For years there has been a sentiment in the civilian world that tourniquets were only to be used as a last resort,” Dr. Mott said. “That’s not true. If done properly, it is absolutely OK to apply a tourniquet for a short time, until the situation stabilizes and you can reassess the patient’s needs. It can save their life.”
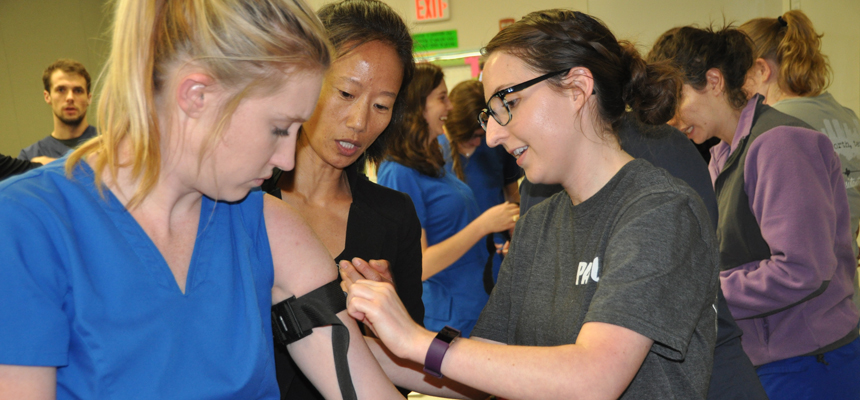
Dr. Mott and Katherine Fogelberg, PhD, DVM, an Assistant Professor in the School of Public Health and U.S. Army veteran, helped PA students practice applying tourniquets, check patients’ distal pulse to make sure it isn’t too loose, and record the time the tourniquet was applied.
Using mannequins, they taught the students to use their hands to sweep blood from the dummies’ chests and backs to identify and apply occlusive dressings to the wounds on the torso.
Dr. Mott has provided TCCC training to UNTHSC police officers and said he hopes to coordinate his efforts with fellow faculty members to spread the word about the White House’s “Stop the Bleeding Coalition,” which is designed to raise awareness of life-saving strategies and provide public access to bleeding control tools.

Social media